Managing the symptoms of long term lung conditions
1. A chronic cough due to irritation of the airways
2. Excess phlegm
3. Increased shortness of breath
4. Wheezing which is the sound produced when air and oxygen are passing through narrowed airways
Long term lung conditions can also affect you in other ways. Patients often experience other challenges as a result of their lung condition:
• tiredness/fatigue
• struggling with daily activities
• anxiety and/or depression
• significant changes in weight
• loss of libido
Unfortunately, lung damage is irreversible. However, there are things you can do to control your symptoms and manage your condition to improve your quality of life.

Managing a flare up
Recognising a Flare Up (exacerbation):
Symptoms are worse than usual during an exacerbation or ‘flare up’ of your lung condition. Being familiar with your usual symptoms can help you to respond quickly if they change. Early recognition and treatment of chest infections will help to prevent further lung damage and speed up your recovery.
If you are having a flare up of your chest symptoms (an exacerbation), please start your Rescue pack immediately if you have one. If you do not have a Rescue pack, contact your GP Practice, nurse or Community Matron immediately.
• increased breathlessness
• increased phlegm volume or thickness
• change in phlegm colour
If you have 2 of the above symptoms, you need to start your rescue pack. If you do not have a rescue pack, you need to book an appointment with your GP or practice nurse.
Other symptoms:
• increased coughing
• increased wheeze
• finding daily activities more difficult than usual
• increased temperature
With these other symptoms, you may benefit from a routine appointment with your GP or practice nurse.
Medication
Taking your medication as prescribed is essential for managing your lung condition. The medications used to treat lung diseases work in many ways and will help to manage your symptoms. The Breathe programme will teach you how to correctly use your inhalers to ensure you are getting the full benefit of the medication.

The main purpose of inhaled therapy is to open airways and reduce inflammation.
There are three main types:
1. Short-acting Bronchodilator or Reliever (opens the airways quickly) These are usually blue and should be taken first to open your airways. The reliever can also be used at any time if you are wheezy, your chest feels tight or you are very breathless. You may also find it useful to use this inhaler before you clear your chest.
2. Long-acting Bronchodilator (keeps the airways open) These should be taken second and can last for at least 12 hours so only need to be used once or twice per day.
3. Steroid or Preventer (keeps airways open and reduces inflammation) These usually contain a low dose steroid and also help to reduce the production of excess phlegm. The preventer should be taken last and you should rinse out your mouth afterwards to prevent thrush.
If your symptoms cannot be controlled with inhalers, your GP may prescribe other medication.
If you have very thick mucus which you find difficult to clear from your chest, your GP may give you Mucolytics. They reduce the thickness of phlegm making it easier to clear. If you are very breathless, there are tablets that can reduce breathlessness which are called Uniphyllin, Phyllicontin or Theophyllin. It is recommended that patients with chronic lung disease have the flu vaccination yearly and pneumonia vaccination once in a life time. If you are still smoking, these medications may not be as effective.
Also note that it can take up to 2 weeks for you to develop immunity from the flu bug for that year and you should not have the jab if you are already unwell or just recovering from illness as this would overload your immune system.
Stopping Smoking
Stopping smoking will reduce the risk of further damage to your lungs and reduce the risk of other health problems such as heart disease and stroke.
If you are still smoking, it is important to start cutting down immediately and make the decision to quit smoking all together as soon as you can. Stopping smoking is very difficult and itis not unusual for patients to try several
times before being able to quit altogether.
Support is available from your General Practitioner, Practice Nurse, Pharmacist at your local chemist or Stop Smoking Liverpool. There are a number of options available to help you quit. Smoking cessation advisors can help you choose the right method for you – this may include the use of Nicotine Replacement Therapy.
For further information – Telephone Smoke Free Liverpool: 0151 374 2535


Nutrition
Eating a balanced diet can help you to maintain a healthy weight. Being overweight can make your breathlessness worse and being underweight reduces your strength and weakens your immune system.
Eating 5 portions of fruit and vegetables a day can provide your body with essential minerals and vitamins to strengthen your immune system, enabling you to fight off chest infections more effectively.
It is recommended to drink 6-8 glasses per day of sugar free fluids such as water, juice, tea or coffee. This can help prevent your phlegm from becoming too thick and difficult to clear from your chest. Good hydration also helps to maintain general health as it allows other organs such as your kidneys to function well. Eating 5 portions of fruit and vegetables a day will help strengthen your immune system, enabling you to fight off chest infections more effectively.
The weather and your health
The environment can have a significant impact on your symptoms. Extreme weather or changes in weather conditions, dust, pollution and damp in the home can make you more breathless. It is important that you carry your inhaler with you at all times and in all conditions.
The Met office is working in partnership with the Department of Health to alert patients during periods of adverse weather and will release alerts for extreme cold, extreme heat, high humidity or pollution on the TV and radio weather forecasts or the Met office website www.metoffice.gov.uk
Tips for cold weather:
• wrap up warm with a hat, scarf and gloves
• cover your nose and mouth with a thin scarf to help warm the air as it enters your lungs
• use central heating and ensure radiators are not blocked by large furniture
• exercise at warmer times of the day if possible eg: midday
• avoid exercise in extremely cold conditions
Tips for warm weather:
• drink plenty of fluids
• wear loose, light clothing
• exercise at cooler times of the day eg: morning or early evening
• use a floor or hand fan
• avoid exercise in extremely hot or humid climates

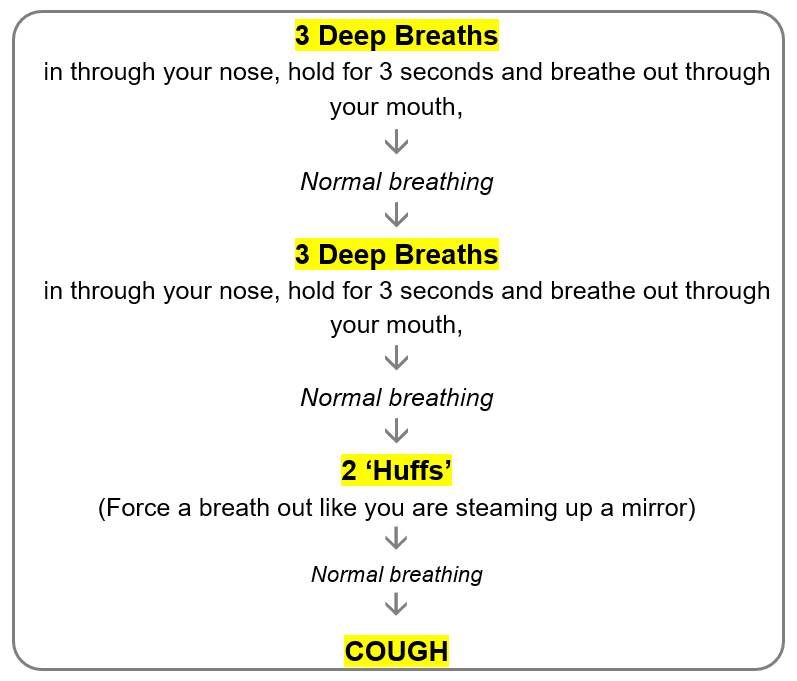
Clearing Your Chest
To help clear phlegm from your lungs you can try the simple cycle of breathing exercises, known as ‘active cycle of breathing techniques’.